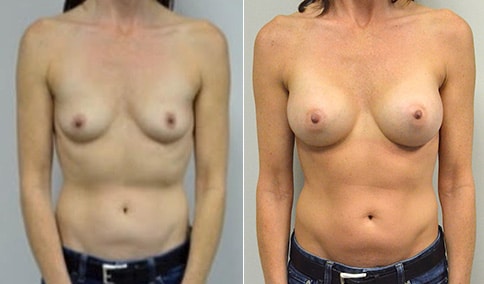
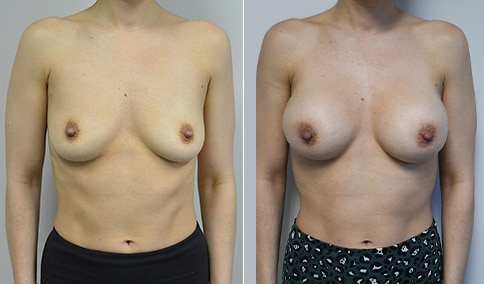
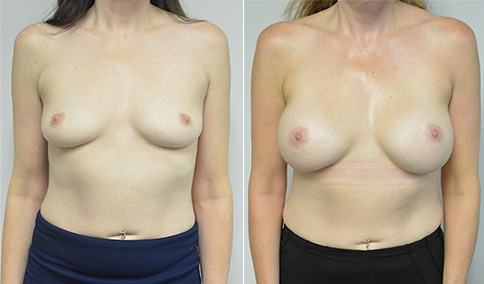
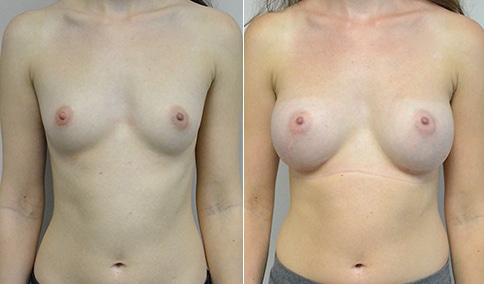
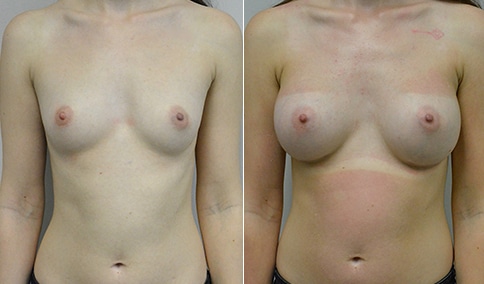
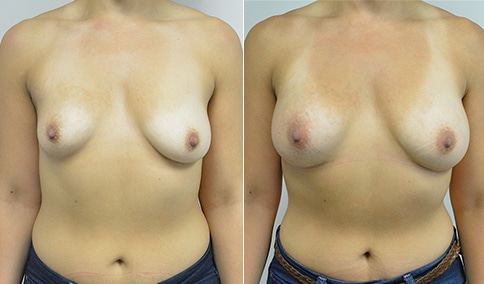
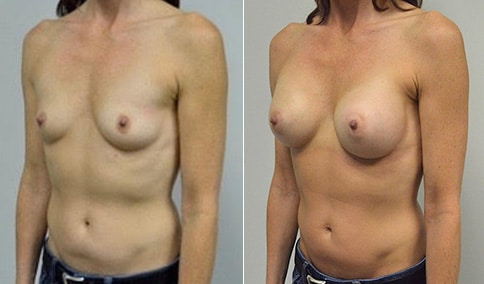
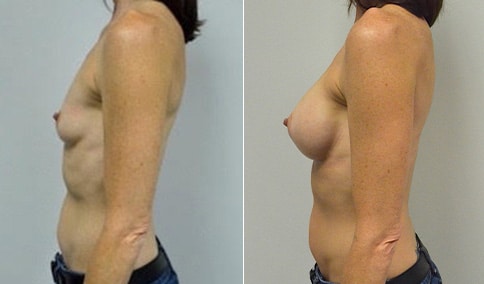
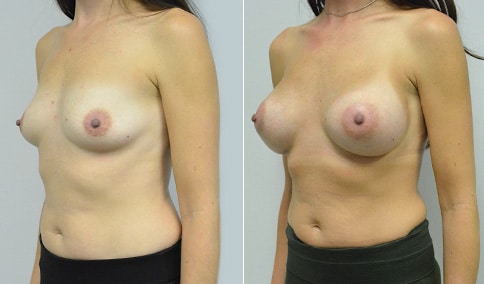
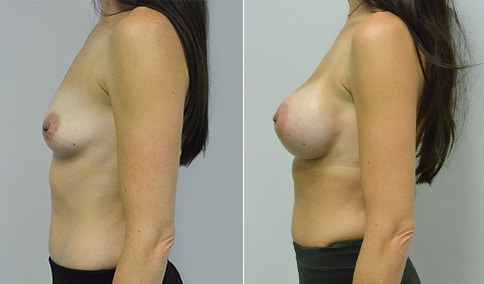
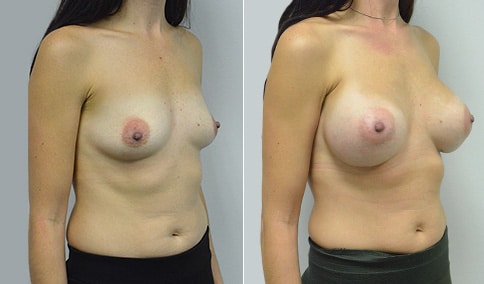
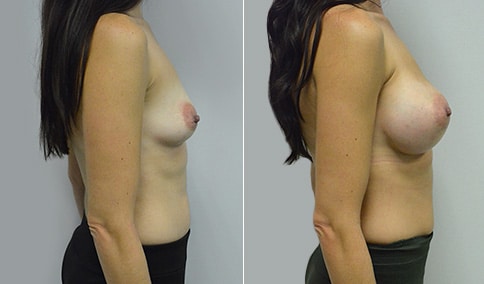
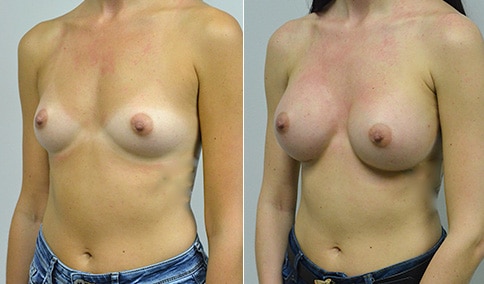
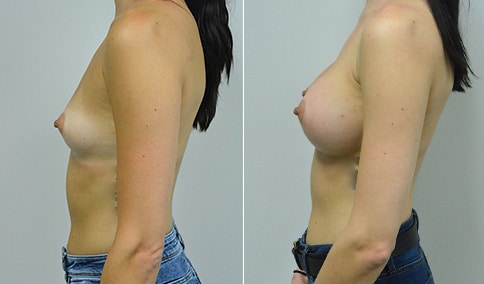
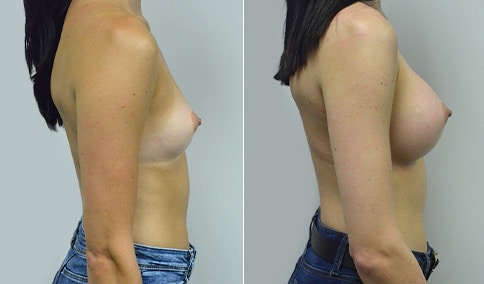
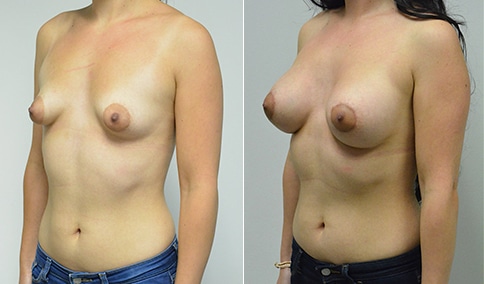
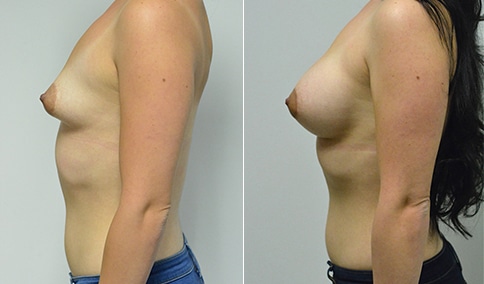
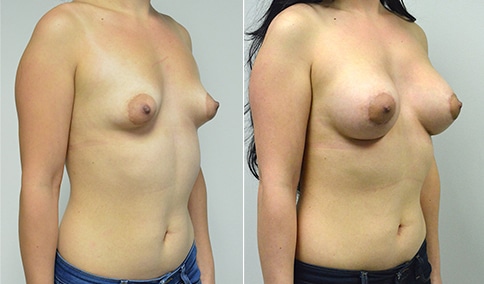
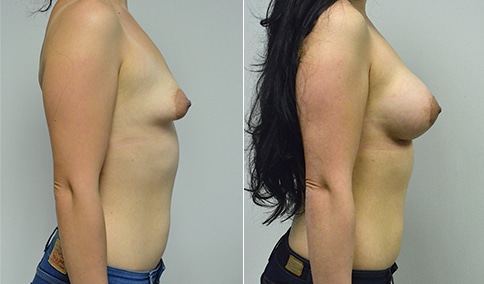
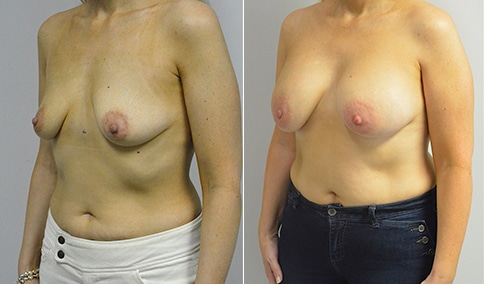
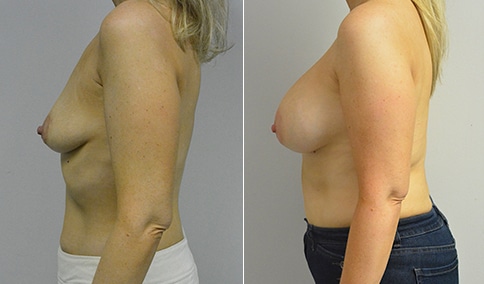
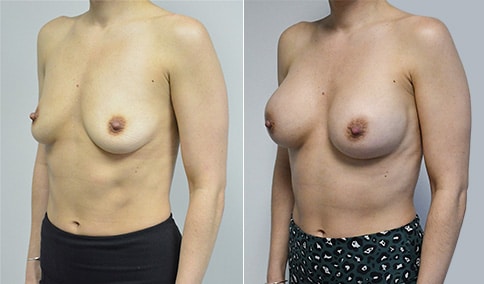
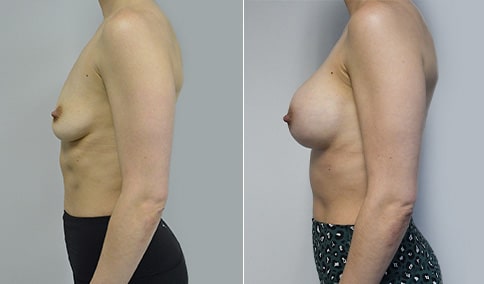
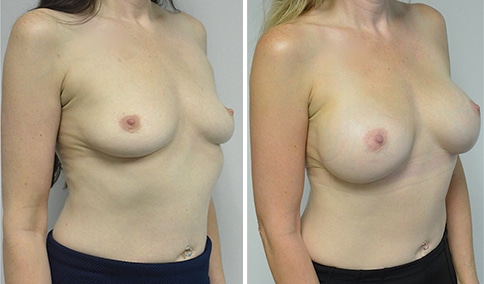
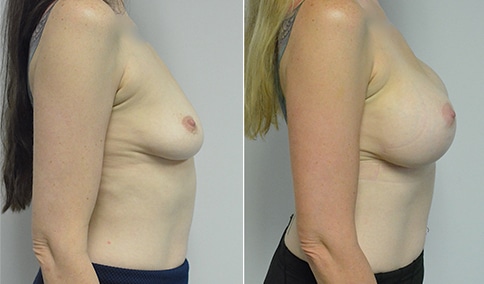
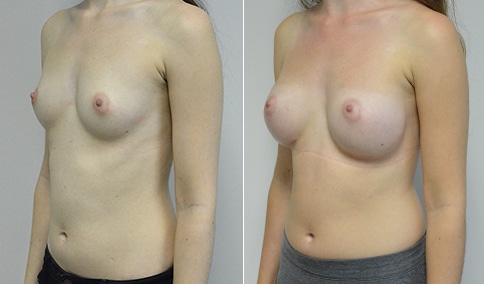
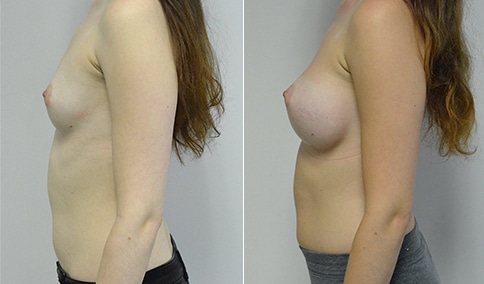
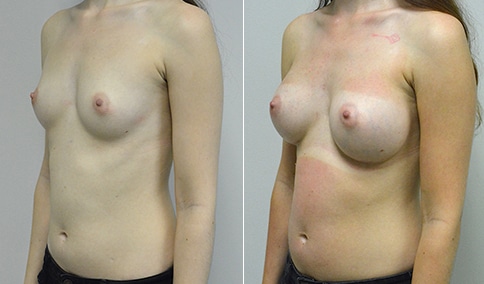
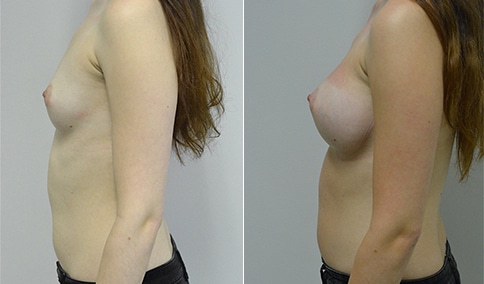
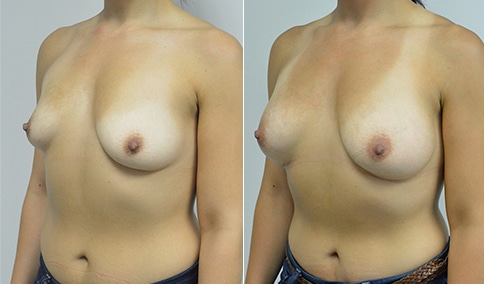
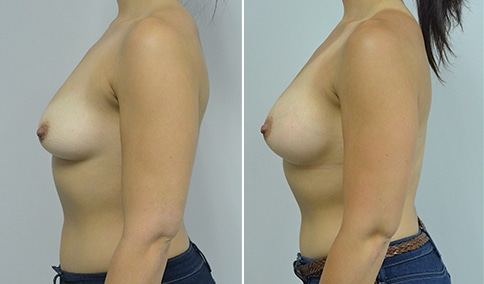
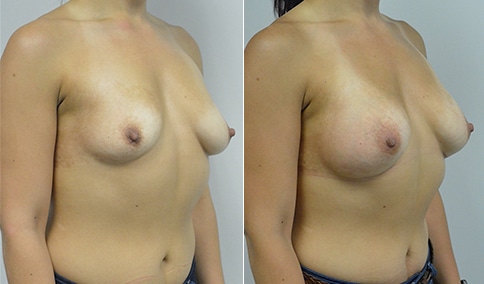
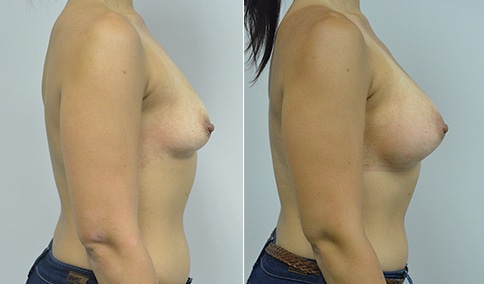
A woman in her early 20’s who describes herself as a 32 a-b cup and would like to be fuller but still relatively natural in appearance. She wanted the Ideal structured saline implant because she did not want to worry about silent rupture but wanted a more natural look and feel than the traditional saline implants. She is shown before and again, 3 months after bilateral partial sub=pectoral placement of the 300 cc Ideal implant filled to 300c, placed through an inframammary incision.
Discussion: She is very petite. When sized for a bra we are taught to measure around the chest just under the breast and add 3 inches- she measures 28” so a 31” bra would be her actual band size if they were made. The base width of her left breast is 11.2 cm. With the Ideal implant the edges are a little firmer and it is best to use an implant base width that is less than the actual breast base width. In a silicone gel implant it is possible to go slightly wider.
In addition, she has a mild pectus excavatum, a hollow in the sternal area that limits the medial placement of the implant. The base width of the 300cc ideal implant is 10.9, so it just fits within the base of her breast. The next larger size is 5 mm wider and would tend to stretch the breast more and appear unnatural. So, as is our usual practice, we want to use the largest implant that we can use that still looks relatively natural and won’t cause problems by overly stretching the breast.






Cosmetic & Plastic Surgery Specialist
"I treat my patients like I would treat
- Jonathan D. Hall, MD, FACSmembers of my own family."
Schedule Consultation