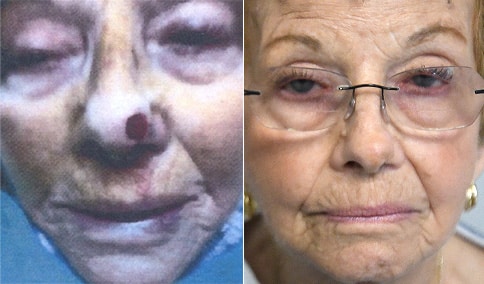
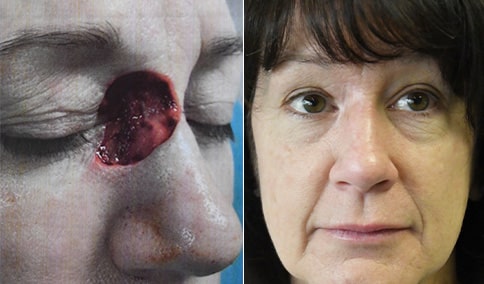
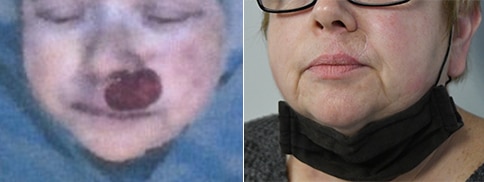
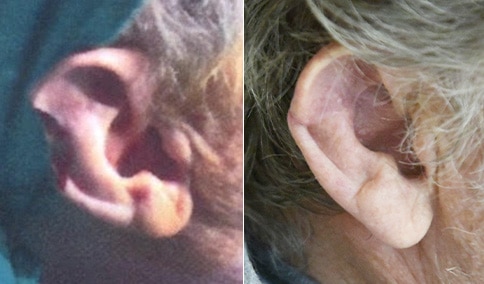
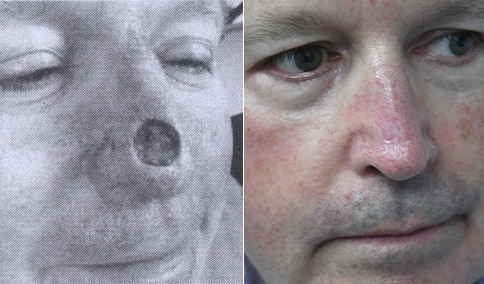
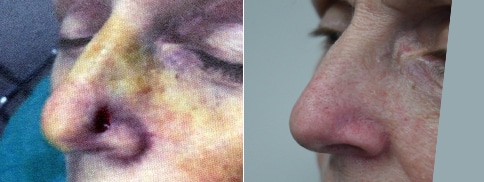
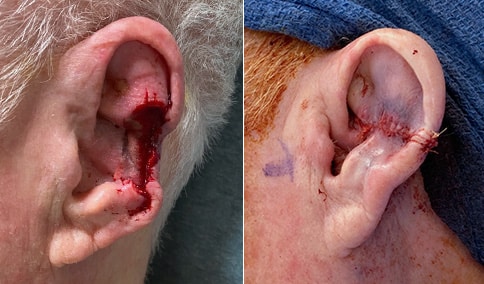
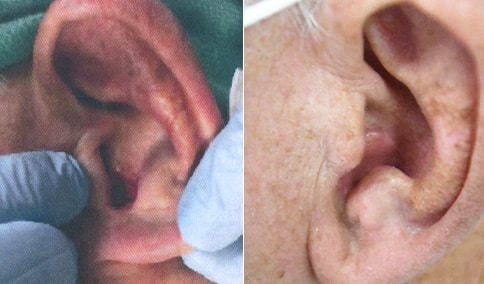
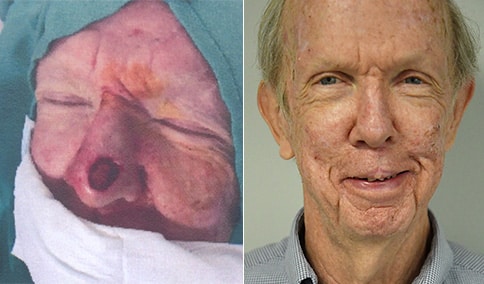
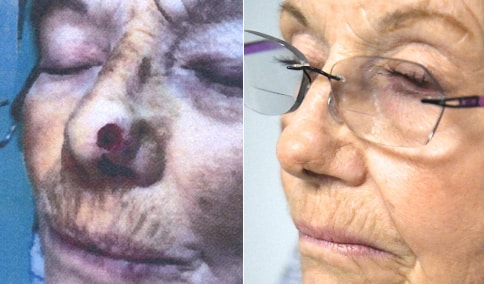
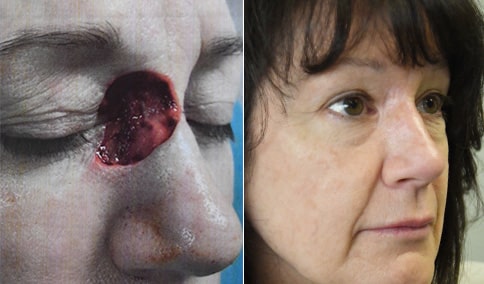
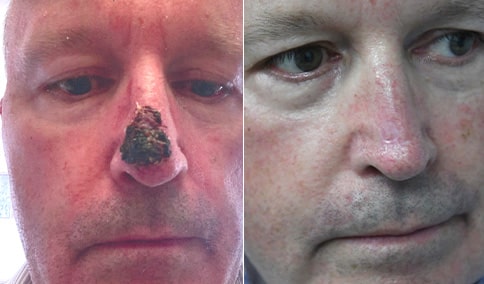
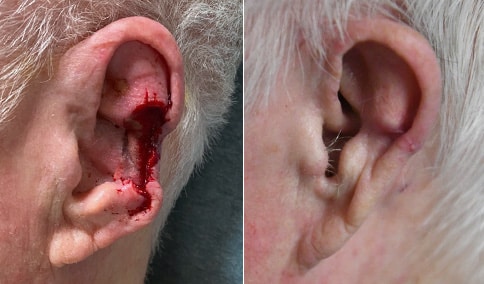
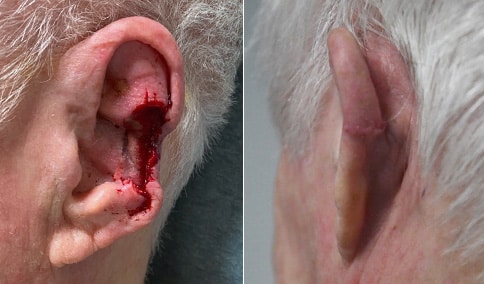
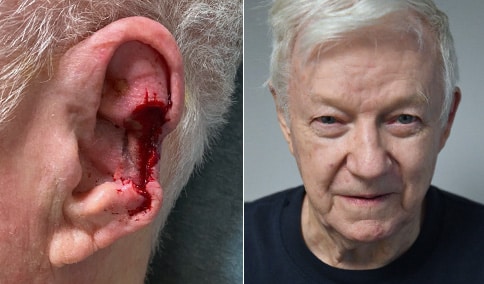
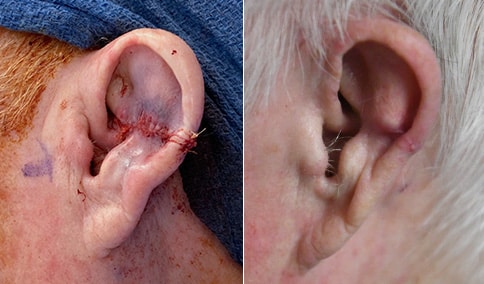
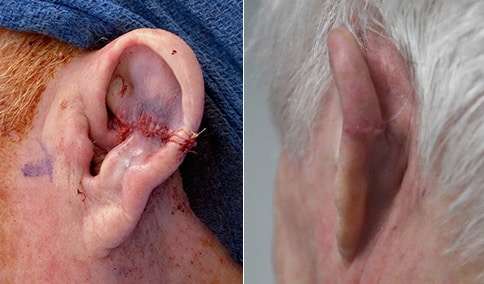
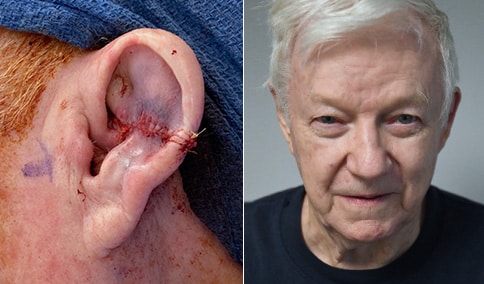
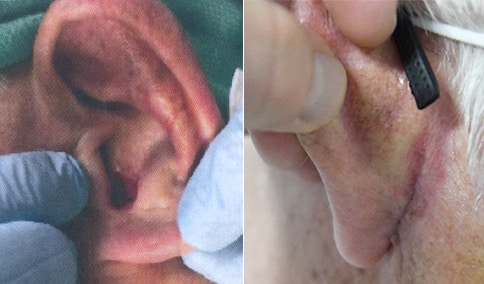
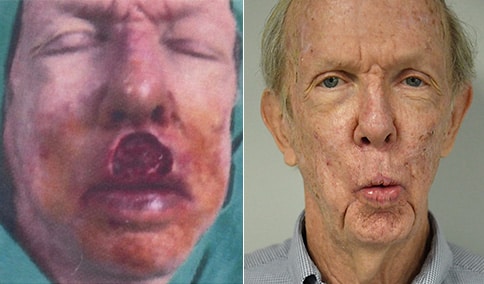
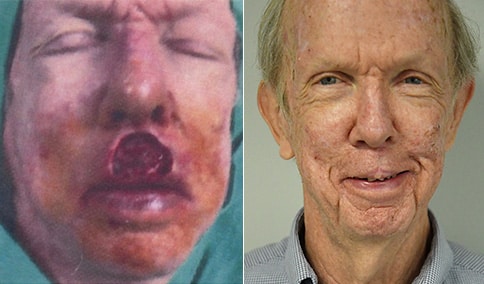
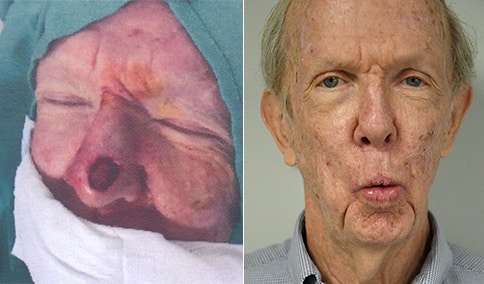
A man in his early 80’s with a large defect of his left ear following Moh’s excision of a squamous cell carcinoma. The ear was reduced and reshaped (“reduction otoplasty”) to give the ear a smaller but still normal appearance. Although the ear is smaller, we do not typically view both ears at the same time and it does not appear deformed. He passes the “little girl” test. The little boys and girls don’t ask their mother “what happened to that man?”
He is shone after his moh’s surgery and immediately after reconstruction.
He is shown again, 4 months after surgery.





Cosmetic & Plastic Surgery Specialist
"I treat my patients like I would treat
- Jonathan D. Hall, MD, FACSmembers of my own family."
Schedule Consultation